We knew it was coming. Rachael was a week past her due date, and just like early causes problems, so too does late delivery. Rachael was to be induced, the child’s entry into the world kickstarted with a combination of oxytocin and “artificial rupture of membranes.” Labor & Delivery at Oregon Health and Sciences University told us to expect a call early in the morning directing us to come in.
Strange to know with such certainty when life will begin, or at least when we say it will begin. Even though our child remained unborn, it was still very much alive. Rachael could feel it moving constantly, and when I placed my hand on her belly I could feel it too. Sometimes when I looked closely I could even see it moving.
For now, officially, there were still three of us. Rachael and Idara and I sat on the back porch and listened to the crickets chirping. I drew a marshmallow with sidewalk chalk and told Idara, who had been calling the unborn child “Marshmallow” for months, that she would soon get to meet it. Idara grabbed her own piece of chalk and drew herself holding its hand. Maybe she’ll be an okay big sister.
A nurse from Labor & Delivery called shortly after 6 a.m. and said they’d be expecting Rachael soon. A few hours later and she was on a slow drip of oxytocin.
 Rachael, shortly after we’d arrived at the hospital.
Rachael, shortly after we’d arrived at the hospital.
Being at the hospital conjured memories from our stay here three years earlier, when Rachael delivered Idara. I was so worried for Rachael’s health and Idara’s health back then that I felt like I was walking around without skin. Even the simplest gestures of kindness would bring me to tears.
Now I felt bored. Rachael’s pregnancy was uncomplicated and the baby appeared to be doing well. It wasn’t a bad boredom, by any means, but it was boredom nonetheless. I expected that Rachael would soon go into active labor, push for an hour or two, and then we’d be done.
We folded origami and played a card game and then waited. And waited. Doctors came in periodically but no one seemed too concerned about her progress. Mostly they left us in peace. Dr. Domingo broke her water shortly after lunch and then we continued to wait.
Progress continued into the afternoon and evening, until Rachael was having powerful contractions continuing to dilate. She handled these well, even though she was clearly in a lot of pain.
I’m reticent to speak too effusively about how Rachael handled the pain that her body created. I was impressed by her strength and focus, how she maintained her breathing through each of her contractions and then collected herself in between. But what if she had cried out and her voice had cracked and she’d said that she couldn’t do it anymore? Would I have thought any less of her?
We treat childbirth as a performance and a battle. Our wives and mothers are our warriors, and we judge them based on how they face it. When Rachael and I talked about this and she wondered whether or not she could handle the pain, I reminded her that when I was cursed with a kidney stone last year I never considered giving it a “natural birth.” I wanted morphine as fast as they could give it to me, and sighed in happy relief once I felt it coursing through my veins. Did anyone judge me for it? Did anyone think me less a man?
Dr. Domingo was there from the beginning and Dr. Hayes appeared later on in the day, around when Rachael started pushing. Other doctors came in and out, but it wasn’t quite like when Idara was born, when the room always felt crowded with residents and attending physicians. A lip on Rachael’s cervix finally receded, which meant that pushing could begin. I think it was a bit after 5 p.m.
This was about Rachael, not me, and so I feel silly mentioning it, but this time around I was proud of myself, too. When Idara was born I didn’t know what to do or how to do it. I wasn’t confident and had a hard time guiding Rachael in the way that she needed to be guided. Thankfully the nurses were there to help, and it was a straightforward delivery.
This time I wanted to be better. I wanted to be able to talk her through her contractions, to help her breath, to advocate for her. And I think I achieved those goals.
 I had to throw in this picture of Idara at Lost Lake because I wasn’t taking pictures while Rachael was pushing and this wall of text was too damn stressful.
I had to throw in this picture of Idara at Lost Lake because I wasn’t taking pictures while Rachael was pushing and this wall of text was too damn stressful.
Unfortunately there wasn’t much time to feel good about myself, because the delivery was failing to progress and Rachael and I began to sense that something was amiss.
Eventually Dr. Domingo and Dr. Hayes said that the baby’s position – face up, possibly even a bit off to the side – was probably preventing further movement down the birth canal. They’d tried to rotate it unsuccessfully. The next thing to try, they said, was an epidural. This would relax the muscles around the birth canal and possibly allow for the baby to be rotated. Rachael delivered Idara without an epidural and planned on the same thing this time around, so this was a significant change in plans. But Rachael had kept an open mind and decided that if the epidural might have the intended effect then it was worth changing course.
A few moments later the anesthesiologist came in and discussed the procedure: Rachael would sit on the edge of the bed and he would insert the epidural needle into her back. It would take several contractions to complete, so Rachael would need to remain seated, breathe through her contractions, and resist the urge to push.
Armed with an epidural, Rachael continued to push for another hour. But the baby did not and would not rotate, and pushing failed to move it further out of her body.
After four hours of pushing, Dr. Hayes and Dr. Domingo said that it was time to consider a Caesarean section, since complications were becoming increasingly likely. It was shortly before 11 p.m.
We discussed the decision briefly with them and then with the two surgeons, Dr. Crane and Dr. Otto, who would perform the procedure. The doctors gave us a moment to discuss the change of plans, but there was nothing to discuss. It was clear that this was the only path forward.
They wheeled Rachael out of the room and I paused them to kiss her and tell her I loved her. I didn’t know how to gauge the risks of what was coming next, but I know that surgery is serious. Dr. Hayes gave me a bunny suit and a hair cover and mask to put on. The nurse said that Rachael would not be returning to this room so I should pack up our things.
Now the room was empty and dark, and so I sat in silence and attempted to regain my strength for what lay ahead. My body was still full of adrenaline. I did my best to ignore the reality of the situation: Rachael going into more or less emergency surgery to deliver the child that was stuck partway down the birth canal.
The operating room was the brightest room I’d ever been in and speakers, somewhere, were playing what sounded like Yo-Yo Ma. Eight or ten people milled about, each focused on their own tasks, with Rachael at the center of it all.
Dr. Hayes guided me to a seat next to Rachael’s head, who I found awake and alert. Her jaw and hands shivering, apparently a side-effect of the medication which now prevented her from feeling much of anything from the chest down. A few minutes after I’d sat down Dr. Hayes asked me if I’d like to watch our child being born. I agreed without a second thought, and so I rose to my feet to peer above the curtain that was blocking Rachael’s view. Dr. Hayes stood behind me with her hands on my hips. “In case you faint,” she said.
The doctors and nurses were moving fast and only saying what was necessary. They were sweating. I couldn’t track all of their movements. I didn’t think that surgery could be so physically demanding.
A moment later, after what appeared to be a tremendous effort on the part of the doctors and nurses, I watched Dr. Crane pull a baby from the opening in Rachael’s belly. He set it on Rachael’s legs and then immediately returned his attention to Rachael.
The baby was lying facing me, and so I could see that it was a boy. I told Rachael, but I was less focused on the sex and more on how limp he looked. When Idara was born the doctor held her up in the air and she cried out. Crying was a sign of life and so I cried, too.
This one did not cry. He was pink – a good sign – but there were no cries, no movement. Later on I’d realize that the calming tones of Yo-Yo Ma had given way to an advertisement for the new Dodge Ram, but for now I just wanted to see my son breathe.
Someone cut the umbilical cord and then someone else, a nurse maybe, lifted him up and began rubbing him with a towel. He began to cry softly a few long seconds later, and his cries grew as the nurse continued to rub him with the towel and flick the bottoms of his feet. Still, they weren’t as loud as they ought to have been, so the nurses continued their efforts – first by suctioning his mouth and throat, and then by applying air pressure via a mask. Within about fifteen minutes they decided that he was doing fine and so placed him in my arms, wrapped in a blanket.
 The first picture of Oren, courtesy Dr. Hayes.
The first picture of Oren, courtesy Dr. Hayes.
The doctors continued their efforts with Rachael. I could see tubes and gauze and needle and thread. I didn’t want to watch too closely since I no longer had Dr. Hayes spotting me, but I saw that the other doctors were still laser-focused on their work and not making any unnecessary conversation.
Thankfully I was now distracted by the baby that was resting in my arms. I could see his hands and feet becoming less and less blue. The nurse listened to his breathing every half an hour and reported good news.
I expected him to sleep, but the room must have been too bright. He would open his eyes briefly and then immediately shut them, as if someone were shining a flashlight directly in his face. I held him down next to Rachael’s face so that she could kiss him and feel his cheek against hers. A nurse helped Rachael express colostrum into a spoon and then handed it to me so I could feed it to him.
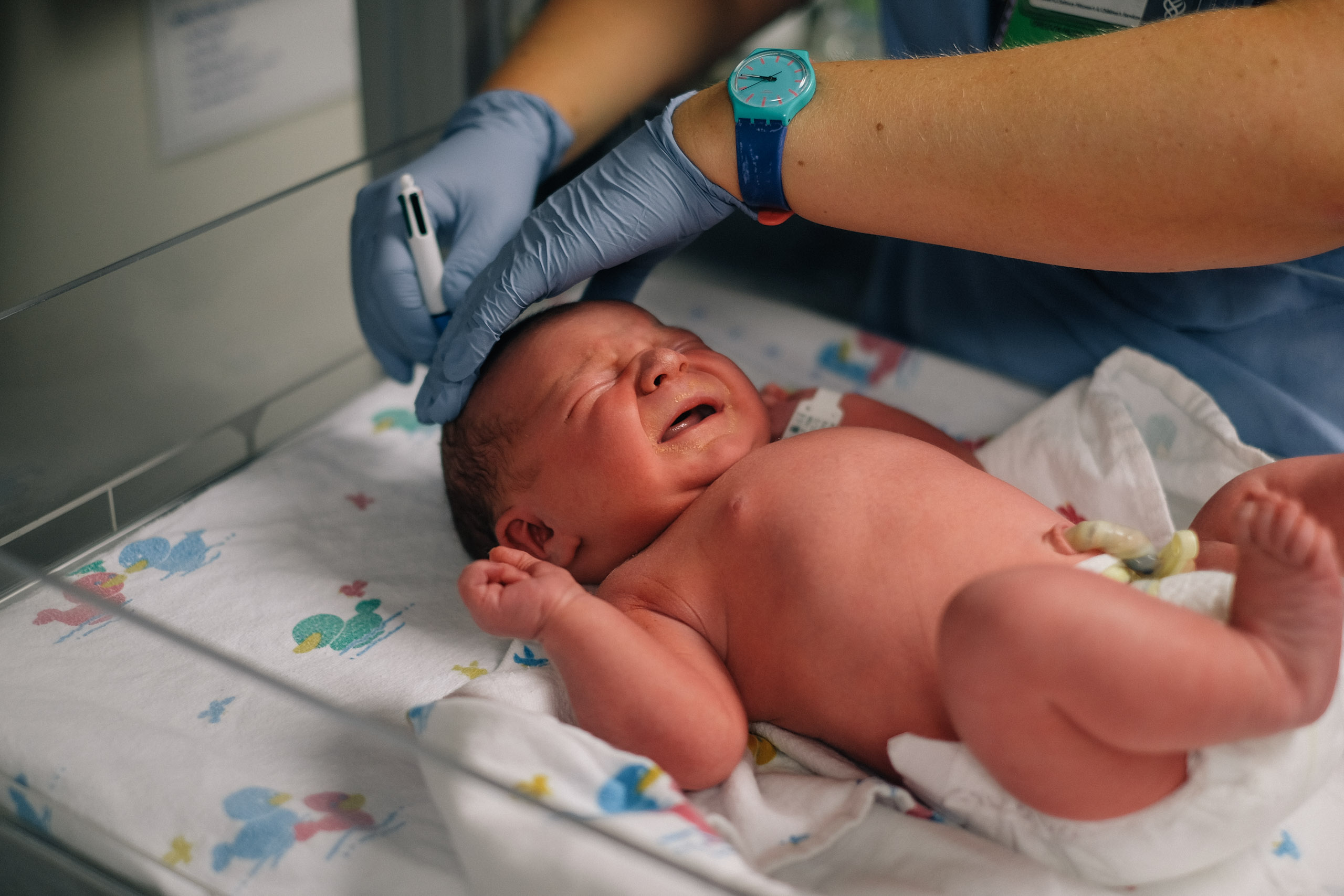 A nurse (whose name I’ve forgotten) recording Oren’s height at 21 inches.
A nurse (whose name I’ve forgotten) recording Oren’s height at 21 inches.
The surgery dragged on. I remember hearing as we went in that most C-sections last about an hour. It had been three. Rachael was trying to sleep so I busied myself by staring down at the baby in my arms.
I tried out a name we’d considered and decided that it fit. Then I started to tell him about his world. About his mother on the operating table a few feet away, about his grandparents and aunts and uncles and cousins. I began to tell him how lucky he was to have such a wonderful big sister, herself brought into this world amidst trying circumstances. This was when I began to cry.
Tears dropped onto my glasses and snot ran into my surgical mask. I simply couldn’t bring myself to talk about Idara to him, and how much I loved her, and how much she would surely love him. I asked for tissue to soak up my tears and a nurse handed me gauze.
I returned to the seat next to Rachael with our son in my arms and asked the anesthesiologist how long it might be before the surgery was complete. He looked over the curtain and said probably an hour or so. Later I would learn about the trauma her organs suffered, and about the bleeding, but for now I simply listened to the tone of the doctors and nurses. I’d never met any of them before today and so didn’t have much to base my suspicions on, but I decided that if they started to sound happy then I could be happy, too.
 Rachael with Oren on her chest.
Rachael with Oren on her chest.
Before long their voices lightened and so did my spirits. Dr. Hayes and Dr. Domingo, who’d overseen the beginning of the delivery, both gave me firm, long hugs and said they’d catch up with us soon. Then I stepped aside as they lifted Rachael off of the operating table and onto the bed that would take her to the recovery room.
Soon after our arrival in the recovery room the surgeon and the anesthesiologist met at Rachael’s bedside and discussed what to do next. When they said that she’d lost approximately two liters of blood I couldn’t help but think of the large soda bottles that would always show up at birthday parties. Two liters is a lot.
The question was whether or not a transfusion was necessary. I remembered seeing a small red cooler with wheels in the operating room, and now it joined us in the recovery room. According to the piece of paper taped to the outside, it contained two liters of blood, type O.
The necessity of the transfusion soon became a moot point. Rachael’s pulse, which had hovered in the 150’s since the completion of the surgery was now inching up toward 180. I watched as she grew increasingly pale. She said she felt faint. Within moments her bedside was crowded with doctors and nurses. The type O blood was hung on a pole and connected to her IV. I watched from the other side of the room as a nurse squeezed the bag empty and then connected another.
Her heart rate soon returned to the 150’s, and then lower still. She started to act herself again, and one by one the extra nurses and doctors filed out of the room until only one remained. It was Jasmine, who’d been with us since a little after 7 p.m. the night before. The early hours of the morning were now upon us, and I looked out the window hoping to see the sun’s first light.
Once Rachael was well enough to hold our son I placed him in her arms so that she could feed him. Breastfeeding was the most challenging part about Idara’s beginning, and so our hearts soared as we saw how vigorously he latched.
My hands were free now so I pulled out my phone and texted my sister. “rachael and baby ok,” I wrote. And it was true.
The rest of the story is beautifully boring. Upstairs to the Mother and Baby Unit. Visits from Idara and grandparents and cousins and an aunt. Nurses whose kindness damn near brought me to tears and others who were all business. Hearing tests and blood draws and bilirubin and blue lights.
 Dr. Andrew Wang checks Oren’s eyes while Idara and I look on. In the background is Dr. Zink and one of our wonderful nurses, Hannah.
Dr. Andrew Wang checks Oren’s eyes while Idara and I look on. In the background is Dr. Zink and one of our wonderful nurses, Hannah.
 Dr. Hayes holds Oren. She played an integral part in Idara’s delivery, too.
Dr. Hayes holds Oren. She played an integral part in Idara’s delivery, too.
We picked a name, Oren, and sat and talked with the doctors and nurses who’d coached Rachael through four hours of labor, and who had cut her open, pulled Oren out, and then put her back together again.
 Idara holds Oren for the first time.
Idara holds Oren for the first time.
We’d checked into the hospital on Thursday morning and finally returned home on Wednesday afternoon, first two, then three, and now four.
 Oren’s grandparents, Gordy and Suellen, and Idara’s caretakers while we spent seven days in the hospital.
Oren’s grandparents, Gordy and Suellen, and Idara’s caretakers while we spent seven days in the hospital.